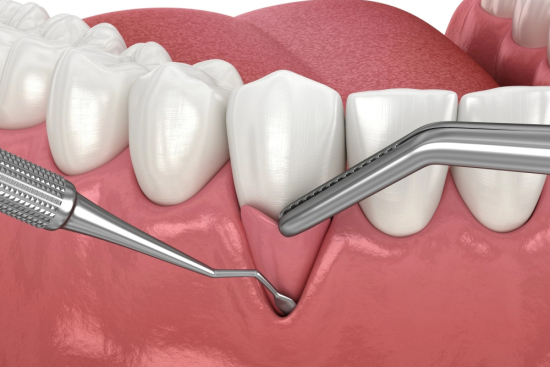
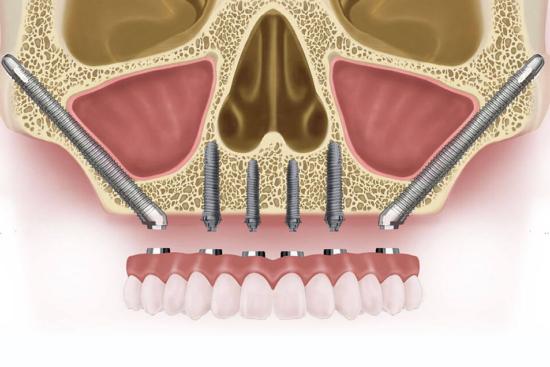
Understanding Your Wisdom Teeth
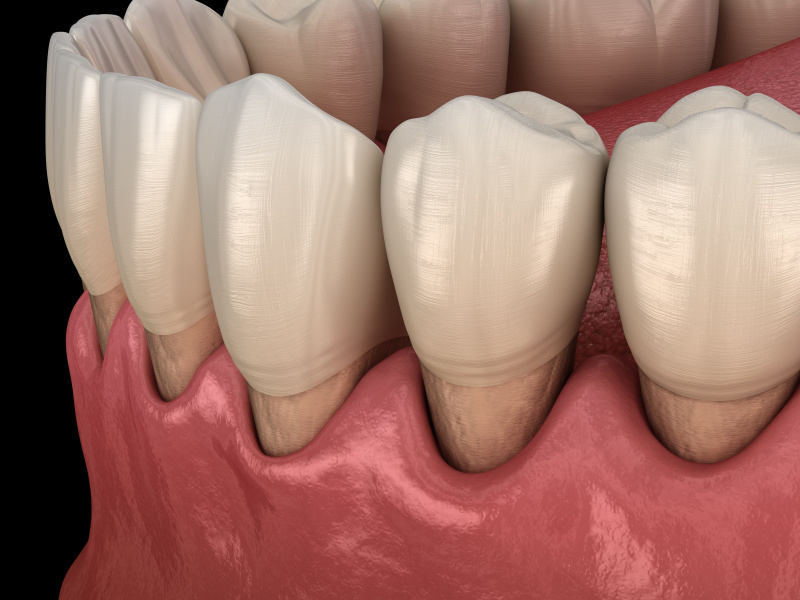
Wisdom teeth are your third molars, the final set of adult teeth to develop. They typically emerge between ages 17 and 30, though some people never develop them at all. Their late arrival creates a common problem: your jaw often lacks sufficient space. When wisdom teeth push through, they frequently cause crowding, pushing adjacent teeth out of alignment and disrupting years of orthodontic work.
Not all wisdom teeth need removal. If yours have erupted fully, sit in the correct position, and you can clean them properly during your daily routine, keeping them may be an option. However, this scenario is relatively rare. Regular dental check-ups remain essential to monitor whether they're causing silent problems like bone loss or decay.
The decision whether to extract or retain wisdom teeth depends on several individual factors: their position within your jaw, degree of eruption, alignment, and overall impact on your oral health. Your dental professional will evaluate these on a case-by-case basis before recommending a course of action.
Why Wisdom Tooth Extraction Becomes Necessary
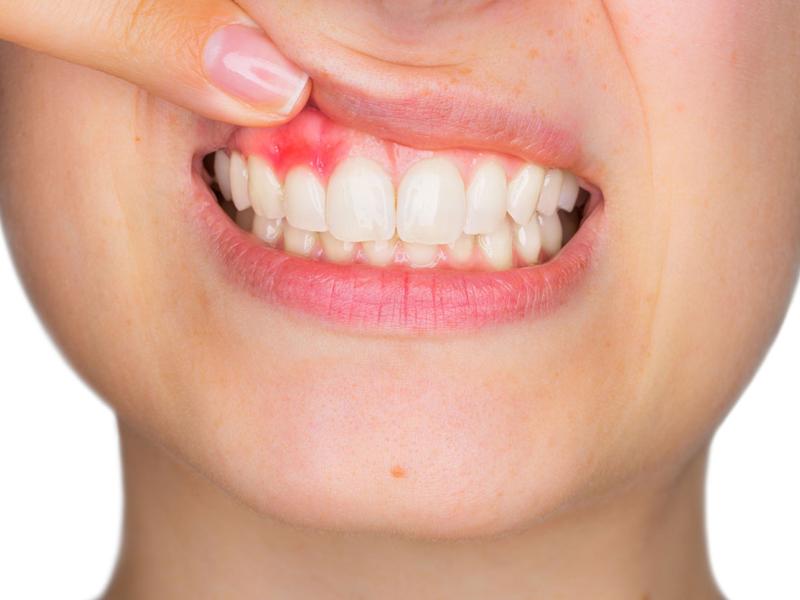
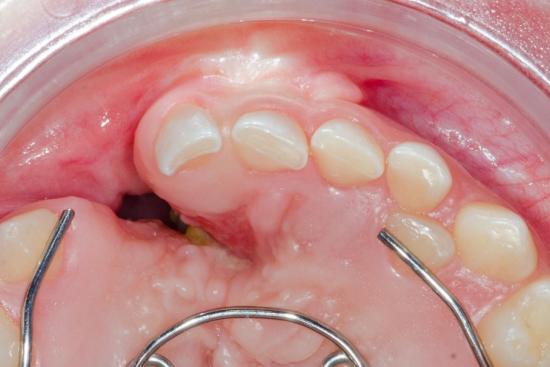
Impacted wisdom teeth rank among the most common reasons for extraction. An impacted tooth fails to erupt properly, remaining partially stuck beneath your gum line or angled against adjacent molars. This creates ideal conditions for bacterial growth, leading to infection, swelling, and pain that can radiate to your ear or jaw.
Chronic overcrowding is another major indicator. Even if your wisdom teeth erupt normally, their eruption pressure can shift your entire dental arch, undoing orthodontic treatment. Some patients experience persistent discomfort around partially erupted teeth, where food debris accumulates beneath the gum flap, causing recurrent inflammation.
Cyst formation occasionally occurs. Your wisdom teeth develop within small sacs; sometimes these fail to drain properly and form cysts that damage surrounding bone and tooth roots. Decay represents a fourth concern. Wisdom teeth sit far back in your mouth, making them difficult to reach with your toothbrush. Even meticulous patients often develop cavities there, which can undermine the tooth's structural integrity.
Your surgical dentist or oral and maxillofacial surgeon will perform evaluation tests, imaging studies, and physical examination to determine your specific situation. X-rays and sometimes 3D CBCT scans reveal the tooth's position, root structure, and relationship to surrounding nerves and sinuses before making an extraction recommendation.
The Extraction Procedure Explained
Wisdom tooth extraction is a surgical procedure requiring specialized expertise. The complexity varies enormously depending on whether your tooth is fully erupted, partially impacted, or severely angled.
Simple extractions occur when the tooth has erupted above the gum line and sits in a straightforward position. Your surgeon applies local anesthesia, uses an elevator instrument to gently loosen the tooth within its socket, then removes it with forceps. The entire process typically takes 15 to 30 minutes for a single tooth. Mild pressure and some tooth movement sensations occur, but pain should not.
Surgical extractions handle impacted or curved teeth. Your surgeon makes an incision in your gum tissue, potentially removes small amounts of surrounding bone to access the tooth, and may section the tooth into smaller pieces for removal. This approach requires more healing time but allows extraction of teeth that cannot be simply pulled out. Surgical extractions usually require general or sedation anesthesia rather than local numbing alone.
Regional anesthesia blocks sensation across your entire lower or upper jaw. General anesthesia renders you unconscious for the duration. The clinics partnered with Turquie Santé can discuss which anesthesia approach suits your comfort level, medical history, and anxiety levels. Patients extracting all four wisdom teeth simultaneously often choose general anesthesia to minimize appointment time and stress.
Modern techniques employed at partner clinics include advanced dental care approaches that prioritize preservation of bone density and nerve function. Piezoelectric instruments sometimes replace traditional drills, reducing heat trauma to surrounding tissue and bone.
Recovery: Timeline and What to Expect
Your recovery unfolds across distinct phases. Immediately after extraction, your surgeon packs the socket with gauze and you'll bite down for 30 to 45 minutes. Slight oozing continues for several hours; this is normal. Some patients see pink-tinged saliva for a day or two.
The first week defines your initial healing phase. Swelling peaks around day two or three, then gradually subsides. Many patients experience moderate pain initially, managed with prescribed pain medication. Ice application during the first 24 hours reduces swelling significantly. Applying ice for 15 minutes, then removing it for 15 minutes, throughout your waking hours yields better results than continuous icing.
Your mouth will feel stiff, especially opening wide. This temporary trismus, or jaw stiffness, improves with gentle stretching exercises after several days. You'll need soft foods: yogurt, soup, pudding, mashed potatoes, and smoothies sustain nutrition without requiring chewing force. Avoid straws for at least a week, as the suction can dislodge clots forming in your extraction sockets.
Bone healing continues for months after your procedure. Three weeks post-extraction, the socket is covered by new soft tissue, though bone filling takes substantially longer. Some surgeons recommend avoiding strenuous exercise for three to five days, though light walking typically poses no risk.
Complete bone remodeling extends several months. This matters if you're considering dental implants later, as bone must achieve sufficient density before implant placement becomes possible.
Managing Post-Extraction Discomfort
Pain control strategies vary by individual. Your surgeon prescribes medications appropriate for your extraction's complexity. For simple extractions, over-the-counter ibuprofen often suffices. Surgical extractions typically require stronger analgesics for the first few days.
Dry socket (alveolar osteitis) occurs when the blood clot protecting your socket dissolves prematurely, exposing bone to air and bacteria. This painful condition develops in roughly 2 to 5 percent of extractions, more frequently in lower wisdom teeth extractions. If you experience intensifying pain after several days of improvement, contact your dentist promptly. They can flush the socket and apply medication to promote clot reformation.
Infection manifests as increasing swelling, pus discharge, fever, or persistent foul odor. While rare with proper surgical technique, infection requires immediate attention. Antibiotics can prevent minor issues from becoming serious complications.
Nerve irritation occasionally causes tingling or numbness in your tongue, lips, or chin. Most nerve sensitivity resolves within weeks, though permanent changes affect a tiny percentage of patients. Your surgeon discusses these risks before the procedure.
Cost and Insurance Considerations
Wisdom tooth extraction costs vary considerably based on complexity and geography. Simple extractions typically range from $200 to $400 per tooth. Surgical removal of impacted teeth can cost $500 to $1,000 per tooth. Extracting all four wisdom teeth ranges from $1,000 to $3,000 or more, depending on impaction severity and your location.
Insurance often covers necessary extractions, especially when impaction causes problems or disease risk. Some plans cover only a percentage after you meet your deductible. Cosmetic extractions, performed solely for orthodontic reasons in a patient without disease, may receive lower coverage or none. Verify your specific coverage before your appointment.
Clinics partnered with Turquie Santé can often provide substantial cost advantages compared to Western European or North American facilities, though the same surgical expertise and post-operative care standards apply.
Alternatives to Extraction
Extraction isn't always inevitable. If your impacted wisdom tooth causes no pain, infection, or damage to adjacent teeth, some surgeons recommend monitoring rather than immediate removal. Regular dental visits with imaging every one to two years track for changes.
For mild overcrowding caused by erupting wisdom teeth, orthodontic treatment can sometimes accommodate them by creating space. This approach works better in younger patients whose jaws still have growth potential. Adults typically have limited room to create new space.
Antimicrobial rinses and improved home cleaning can manage mild inflammation around partially erupted teeth. If your wisdom tooth remains consistently asymptomatic and imaging shows no bone loss or decay, conservative management remains valid.
Questions to Ask Your Dentist
Before committing to extraction, clarify your surgeon's reasoning. Specifically ask whether your tooth requires immediate extraction or allows monitoring. Request detailed imaging explanations: point out the tooth's exact position, angle, and any visible decay or damage.
Discuss anesthesia options and what each entails for your situation. Ask about typical recovery duration for your specific case and what activities you'll need to modify. Confirm your surgeon's experience with wisdom tooth extraction and whether they perform these regularly.
Understand the infection and complication rates at your specific clinic, not general statistics. Ask what happens if complications arise, whether your surgeon will manage them at no additional cost, and how they handle patient emergencies after hours.
If implant replacement interests you later, ask about bone density preservation during extraction and whether any bone grafting might serve your future needs. The clinics affiliated with Turquie Santé can connect you with experienced oral surgeons who address these questions thoroughly before your procedure.