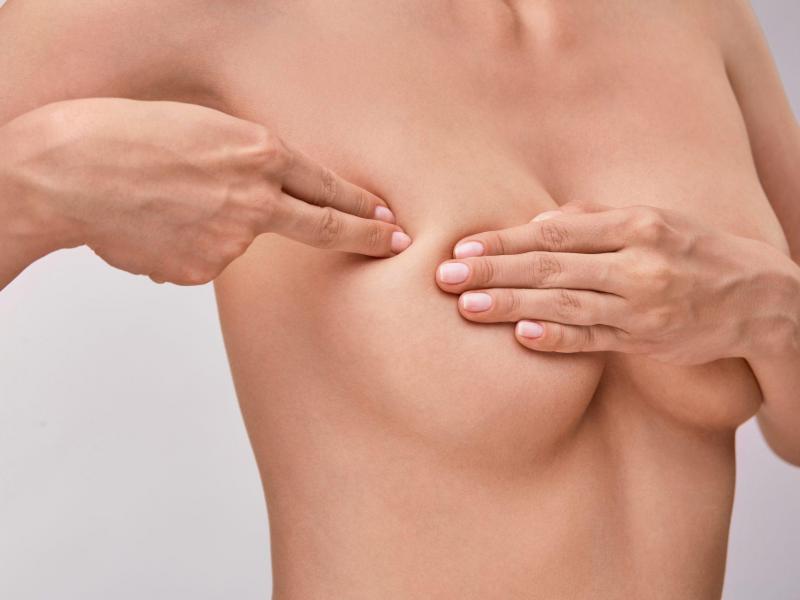
Breast self-examination represents one of the simplest yet most effective ways for women to stay informed about their breast health. Regular monthly checks allow you to become familiar with how your breasts normally look and feel, making it easier to spot any changes that might require medical attention. While no single screening method catches every breast cancer at its earliest stage, combining self-examination with other approaches significantly increases your chances of detecting abnormalities early, when treatment outcomes tend to be more favorable.
The goal of self-examination isn't to diagnose cancer. Rather, it's about developing body awareness. Any changes you notice, whether a lump, dimpling, discharge, or skin texture alteration, should prompt a conversation with your gynecologist or healthcare provider. Early professional evaluation is what matters most.
When and How to Perform Your Monthly Check
Timing your self-examination correctly makes a real difference. Women who menstruate should perform their check about a week after their period starts, when hormonal swelling has typically decreased. This is when your breasts are least tender and lumps are easier to detect. For women past menopause or those with irregular cycles, picking the same day each month, perhaps the first of the month or your birthday, creates a helpful routine that's easy to remember and maintain.
Your first self-examination serves a crucial purpose: establishing your baseline. Breast tissue naturally has a lumpy, textured quality. This glandular texture varies significantly between women, and it can feel different in various parts of the breast. Some areas may feel more granular, others denser. By doing an initial careful examination, you're essentially creating a mental map of what's normal for you, which makes spotting actual changes much simpler in months to come.
The Visual Inspection Phase
Start by undressing and standing in front of a mirror in good lighting. This first part requires no touching, just observation. Look at your breasts from several angles: arms at your sides, arms raised above your head, and hands pressed against your hips. Notice the size, shape, and symmetry of your breasts. Some asymmetry is entirely normal, most women's breasts aren't perfectly matched.
During this visual step, watch for skin changes that seem new or unusual. These might include:
- Dimpling or puckering of the skin (similar to orange peel texture)
- Redness, irritation, or unusual warmth
- Inversion of a nipple that was previously flat or protruding
- Scaling or crusting around the nipple
- Any visible bulging or contour irregularities
Skin changes can sometimes indicate underlying issues, so documenting what you see helps your doctor if you need to follow up. If you're visually tracking changes month to month, taking photos in the same lighting and position can be surprisingly helpful for remembering how things looked before.
Palpation: The Hands-On Examination
Now comes the tactile part. Lie down on your back on a bed or firm surface. This position flattens the breast tissue against your chest wall, making it easier to feel anything abnormal. Some women prefer to do part of the exam in the shower, where wet skin allows fingers to glide more easily, though this requires a bit more care.
Use the flat pads of your three middle fingers (not your fingertips, which are too sensitive) to systematically examine each breast. Work methodically using one of two patterns: the circular method or the vertical strip method. Many women find success with vertical strips, starting at the collarbone and moving downward toward the lower breast and chest wall, then shifting slightly inward and repeating, until you've covered the entire breast from the armpit to the breastbone.
Apply varying pressure levels during palpation. Begin with light touch to examine the skin and tissue just beneath it. Then use medium pressure to feel deeper. Finally, apply firm pressure to reach the tissue closest to the chest wall. Each layer matters. A lump in the superficial tissue can feel quite different from something deeper, and your doctor will want to know about both.
Don't forget the often-overlooked areas. The upper, outer portion of each breast, extending toward the armpit, is where many cancers develop. This region requires thorough attention. Also examine the area directly under the nipple and areola, as well as the fold of skin beneath the breast. Some tissue naturally extends quite far toward the armpit, so make sure your exam reaches that far.
What You're Actually Feeling For
Normal breast tissue has a somewhat lumpy quality that many women describe as 'nodular' or 'granular.' This is completely ordinary and not a sign of disease. What you're looking for is something that feels distinctly different from the surrounding tissue. This might be a hard lump with clear borders, an area of unusual thickness compared to the opposite breast, or firmness that seems localized and separate from the general texture around it.
Dimpling visible when your arm is raised, puckering that wasn't there before, or a sensation of tissue being drawn inward can indicate something worth checking. Discharge from the nipple is also worth reporting to your doctor, especially if it appears spontaneously (without squeezing the nipple) or comes from only one breast.
It's worth noting that hormonal fluctuations throughout your cycle will cause breast tissue to change naturally. Swelling, tenderness, and increased lumpiness in the days before your period is normal. This is exactly why timing your self-exam for a consistent point in your cycle matters, you're always examining tissue in a similar hormonal state.
Don't Neglect the Axillary Area
The armpit region contains breast tissue that extends farther than most women realize. Using the same palpation technique with flat finger pads, examine the area where your breast tissue meets your armpit, extending up into the hollow. Lymph nodes in this region can occasionally swell for various reasons, and your doctor should know if you've noticed changes there.
When to Seek Professional Evaluation
Finding something during your self-examination shouldn't cause panic, but it should prompt action. Schedule an appointment with your gynecologist or primary care physician if you notice any of the following: a new lump or mass, unusual skin changes, spontaneous nipple discharge, unexplained pain, or anything that simply feels different to you compared to your baseline.
Your doctor can determine whether what you've found warrants further imaging such as breast biopsy or gynecological evaluation. If you're concerned or if your physician recommends additional screening, the clinics partnered with Turquie Santé can provide access to specialists experienced in breast health assessment and advanced diagnostic techniques.
Combining Self-Exam with Other Screening Methods
Self-examination works best as part of a comprehensive approach. Depending on your age, family history, and risk factors, your healthcare provider may recommend mammography, ultrasound, or MRI at specific intervals. For some women, especially those with higher risk profiles, more frequent or advanced imaging becomes important. Self-awareness between scheduled screenings adds an extra layer of vigilance.
Women with dense breast tissue, a family history of breast cancer, or those carrying genetic mutations may benefit from enhanced screening protocols. Your doctor can help you understand your personal risk and determine the optimal combination of self-examination and professional screening for your situation.
Practical Tips for Consistency
Make self-examination part of your routine. Some women do it right after their period ends. Others set a phone reminder on the first day of each month. Keeping a simple calendar mark or note can help you track whether you've done your monthly check. There's no penalty for doing the exam twice in a month if you're unsure, but consistency really does make it easier to spot actual changes rather than normal variation.
If you find it difficult to remember or feel uncertain about your technique, don't hesitate to ask your doctor to walk you through it during a regular visit. They can show you what normal tissue feels like on your breasts specifically and point out areas that might need extra attention based on your individual anatomy.
Common Concerns About Self-Examination
Many women worry they'll miss something or incorrectly identify normal tissue as abnormal. This is precisely why self-examination is not meant to be diagnostic, it's meant to empower you with awareness. False alarms are actually quite common and completely normal. The vast majority of lumps found during self-exam turn out to be benign cysts, fat deposits, or normal glandular tissue. Getting them checked by a professional isn't wasted effort; it's responsible health management.
Some women become anxious about their self-exams, particularly if they have a family history of breast cancer. If self-examination causes excessive worry, discuss this with your healthcare provider. They can help you find an approach that supports your wellbeing rather than creating stress. For some individuals, focusing on regular professional screenings may be more helpful than frequent self-checks.
Knowledge Is Your First Defense
Breast cancer risk varies substantially based on genetics, lifestyle, reproductive history, and hormone exposure. While no screening method is perfect, knowing your breasts well gives you the advantage of noticing when something truly changes. That early awareness, combined with prompt medical evaluation when needed, remains one of your most important tools for protecting your breast health.
Take time to learn your baseline, stay consistent with monthly checks, and don't hesitate to bring any concerns to your healthcare provider. Your vigilance, paired with professional medical judgment, creates the best possible chance of catching any problems early.