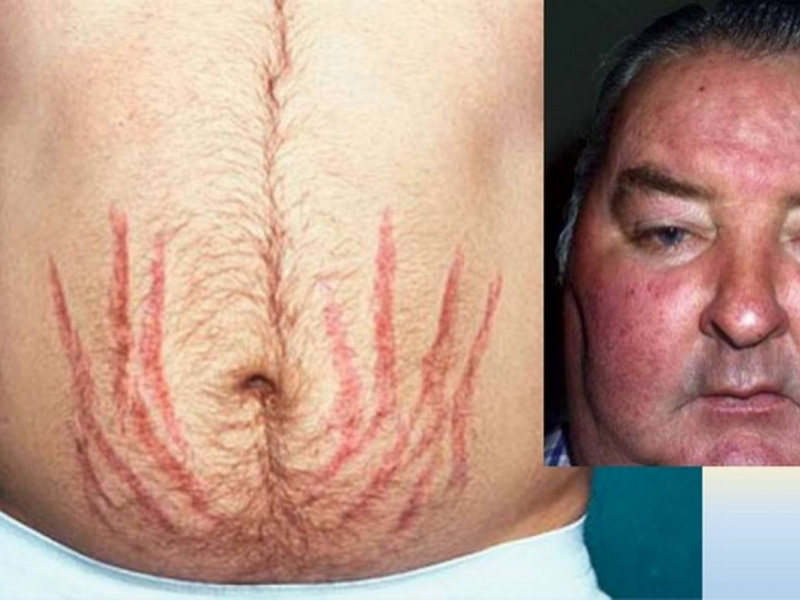
Persistent fatigue, puffy face, progressive weight gain without clear cause. These signs often go unnoticed, attributed to stress or aging, yet they can signal something far more serious: Cushing's syndrome. This rare hormonal disorder silently disrupts multiple organ systems, with cardiovascular consequences that develop insidiously and demand urgent attention.
The mechanism is deceptively simple. Cortisol, your body's primary stress hormone, regulates blood pressure, glucose metabolism, and inflammatory responses. In healthy amounts, it sustains daily function. In excess, accumulated over months or years, cortisol acts as a metabolic poison, systematically damaging the heart and blood vessels.
Understanding Cushing's Syndrome and Its Origins
Cushing's syndrome represents a state of chronic, pathological cortisol excess. Unlike the normal daily fluctuation in cortisol levels (highest in early morning, dropping toward evening), Cushing's syndrome obliterates this rhythm. Cortisol remains elevated constantly, bathing tissues in a hormone that was never meant to persist at such concentrations.
The syndrome emerges from two distinct pathways:
Endogenous sources (internal production) account for most cases. A benign pituitary adenoma secreting excessive adrenocorticotropic hormone (ACTH) drives the adrenal glands into overdrive. This specific presentation, called Cushing's disease, comprises roughly 70% of endogenous cases. Alternatively, a primary adrenal tumor might produce cortisol independently, bypassing pituitary control entirely. Rarer still, ectopic ACTH secretion occurs when a small cell lung cancer or other malignancy produces ACTH from outside the pituitary-adrenal axis, flooding the body with hormone signals.
Exogenous sources (external/iatrogenic) arise from prolonged high-dose corticosteroid therapy. Patients treated for autoimmune conditions like rheumatologic disease, chronic inflammatory bowel disease, or severe respiratory conditions may receive synthetic glucocorticoids for months or years. The body suppresses its own cortisol production, then when medication is withdrawn too rapidly or doses remain too high, Cushing's syndrome can develop.
The Cardiovascular Crisis: How Excess Cortisol Damages Your Heart
Elevated cortisol directly and indirectly harms cardiovascular tissue through multiple pathways. This isn't theoretical damage. The effects are measurable, progressive, and potentially irreversible without treatment.
Hypertension emerges early. Cortisol increases sodium reabsorption in the kidneys and enhances the sensitivity of blood vessels to catecholamines (adrenaline and noradrenaline). Patients typically develop moderate to severe hypertension, often resistant to standard antihypertensive therapy. Blood pressure readings of 160/100 mmHg or higher are common. This sustained elevation strains the heart's left ventricle, thickening the muscle wall (left ventricular hypertrophy). Over time, the thickened, stiffened ventricle struggles to relax and fill properly, potentially progressing to diastolic dysfunction and heart failure.
Electrolyte disturbances compound the problem. Excess cortisol mimics aldosterone, causing potassium loss and sodium retention. Hypokalemia weakens cardiac myocytes and predisposes to dangerous arrhythmias, from atrial fibrillation to ventricular ectopy.
Metabolic derangement accelerates atherosclerosis. Cortisol is a catabolic hormone that breaks down lean tissue and promotes central fat deposition. Patients gain weight, particularly around the trunk and face (the characteristic "moon face" and "buffalo hump"). This visceral adiposity is not cosmetic; it is metabolically active tissue that secretes inflammatory cytokines and impairs insulin signaling.
Insulin resistance develops rapidly. Studies show that 50-80% of Cushing's syndrome patients manifest glucose intolerance or frank diabetes mellitus. The combination of hyperglycemia, dyslipidemia (elevated triglycerides, reduced HDL cholesterol), and central obesity constitutes metabolic syndrome, a powerful accelerator of coronary artery disease. Endothelial dysfunction precedes visible atherosclerotic lesions by years, allowing plaque formation to progress silently until angina or myocardial infarction occurs.
Lipid abnormalities worsen. Cortisol increases hepatic very-low-density lipoprotein (VLDL) production and impairs cholesterol clearance. LDL cholesterol may be only modestly elevated, yet the particle composition shifts toward smaller, denser particles, which are more atherogenic. HDL cholesterol, the protective form, drops.
Prothrombotic state and inflammation. Excess cortisol suppresses fibrinolysis and increases circulating fibrinogen and Factor VIII, creating a hypercoagulable state. Paradoxically, cortisol is immunosuppressive overall, yet it drives systemic inflammation through dysregulated monocyte and endothelial function. Inflammatory markers (C-reactive protein, IL-6) elevate, promoting endothelial damage and plaque destabilization.
Direct myocardial effects. Cortisol excess damages the myocardium beyond hypertrophy. Collagen deposition increases, promoting fibrosis. Apoptosis (cell death) of cardiac myocytes accelerates. Some patients develop cardiomyopathy with severely reduced ejection fraction, a complication that may persist even after successful treatment of the underlying cortisol excess.
Clinical Presentation and Cardiovascular Symptoms
Patients rarely present with a clear "cardiovascular" complaint that immediately raises suspicion of Cushing's syndrome. Instead, the picture is often muddled, delayed by months or years.
Early signs include generalized fatigue, muscle weakness (from protein catabolism), and easy bruising. The skin becomes thin and fragile; purplish stretch marks (striae) appear on the abdomen, flanks, and breasts. Mood disturbances, depression, anxiety, even psychosis in severe cases, occur in over 50% of patients. Women may experience amenorrhea or severe menstrual irregularities; men may develop erectile dysfunction.
Cardiovascular symptoms arrive later, often masked. Dyspnea on exertion might be attributed to deconditioning or obesity rather than heart failure. Palpitations occur, sometimes from atrial fibrillation triggered by electrolyte imbalance. Chest discomfort or angina may develop insidiously, recognized only in retrospect after a cardiac event.
Hypertension itself may be asymptomatic, detected only on routine screening. Some patients experience headaches and visual disturbances. Those with pituitary adenomas may develop visual field defects (bitemporal hemianopsia) if the tumor compresses the optic chiasm, a sign of mass effect rather than hormonal toxicity.
Diagnostic Pathways and Confirmation
Suspicion must precede diagnosis. A patient with hypertension refractory to three or more antihypertensive agents, especially if young or obese, warrants endocrine evaluation. The combination of hypertension, diabetes, and hypokalemia in a single patient is a red flag.
24-hour urinary free cortisol (UFC) remains the screening gold standard. Normal values are typically 20-90 μg/24 hours; in Cushing's syndrome, values often exceed 2-3 times the upper limit. Two elevated 24-hour UFC measurements suggest the diagnosis, though a single normal result does not exclude it (mild cases may fluctuate).
Late-night salivary cortisol offers convenience and sensitivity. Cortisol normally suppresses in the evening; in Cushing's syndrome, this suppression is lost. Samples collected at 11 PM show cortisol levels typically >5 ng/mL, compared to <3 ng/mL in healthy controls.
Low-dose dexamethasone suppression test (LDDST) exploits the normal feedback mechanism. Dexamethasone, a synthetic glucocorticoid, suppresses ACTH and cortisol in healthy individuals. In Cushing's syndrome, this suppression fails. A plasma cortisol >5 μg/dL after 1 mg of dexamethasone at midnight indicates cortisol autonomy.
Once Cushing's syndrome is confirmed, the source must be identified. Plasma ACTH distinguishes ACTH-dependent (pituitary or ectopic) from ACTH-independent (adrenal) forms. MRI of the pituitary reveals adenomas in 80-90% of Cushing's disease cases. CT or MRI of the adrenals identifies primary adrenal pathology. Ectopic ACTH sources may require chest CT, octreotide scintigraphy, or PET imaging.
Cardiovascular Complications and Prognosis
Left untreated, Cushing's syndrome carries severe morbidity. Mortality increases 2-4 fold compared to age-matched controls, primarily from cardiovascular causes. Myocardial infarction, sudden cardiac death from arrhythmia, and heart failure account for the majority of deaths.
Stroke risk escalates due to hypertension and the prothrombotic state. Atrial fibrillation, present in 10-15% of Cushing's patients, further elevates stroke risk and requires anticoagulation.
Cardiomyopathy develops in 5-10% of patients with severe, prolonged hypercortisolism. The ejection fraction may drop below 40%, and symptoms of heart failure, orthopnea, paroxysmal nocturnal dyspnea, peripheral edema, emerge. Reassuringly, some improvement in ejection fraction occurs after successful cortisol normalization, though residual dysfunction may persist.
Sudden cardiac death from malignant arrhythmias represents a feared complication, particularly in those with severe hypokalemia, left ventricular hypertrophy, and prolonged QT interval on ECG.
Treatment Strategies and Cardiovascular Recovery
Surgical intervention is the primary treatment for endogenous Cushing's syndrome. Transsphenoidal pituitary adenomectomy achieves cure in 70-90% of Cushing's disease cases when performed by experienced neurosurgeons. Adrenalectomy is definitive for adrenal adenomas and carcinomas. Resection of ectopic ACTH sources (lung cancers, carcinoids) is pursued when feasible.
Medical therapy bridges the gap before surgery or manages inoperable cases. Mitotane, an adrenolytic agent, slowly reduces adrenal steroid synthesis but requires months to achieve effect. Metyrapone and ketoconazole inhibit 11-beta-hydroxylase and 17-alpha-hydroxylase, respectively, reducing cortisol production acutely. Mifepristone, a glucocorticoid receptor antagonist, acts peripherally and may improve metabolic parameters rapidly. Newer agents like osilodrostat target the enzymes of steroidogenesis with greater specificity.
For iatrogenic Cushing's syndrome, cautious corticosteroid tapering is essential. Abrupt withdrawal risks acute adrenal insufficiency and can paradoxically worsen inflammation in the underlying disease. Gradual dose reduction, often over weeks to months, allows the suppressed pituitary-adrenal axis to recover.
Cardiovascular monitoring and management. Cardiology evaluation is advisable for all Cushing's patients, particularly those with hypertension, symptoms of ischemia, or arrhythmias. Electrocardiography and echocardiography assess left ventricular function, wall thickness, and valve integrity. Stress testing or coronary angiography may be warranted if angina is present. Aggressive blood pressure control during the diagnostic and treatment phase prevents further left ventricular damage; typically, multiple antihypertensive agents are needed until cortisol is normalized.
Potassium supplementation corrects hypokalemia and reduces arrhythmia risk. Anticoagulation prevents thromboembolic complications in those with atrial fibrillation or immobility. Lipid-lowering therapy (statins) addresses dyslipidemia, though the most dramatic improvements occur after successful cortisol suppression.
Glucose control requires insulin or agents suited to insulin-resistant states. Post-treatment, many diabetic patients experience partial or complete remission of hyperglycemia.
Recovery Timeline and Long-Term Outcomes
Cardiovascular improvement unfolds over months to years, mirroring the timeline of tissue remodeling. Blood pressure begins to fall within weeks of cortisol normalization but may not reach target for 3-6 months. Some hypertension persists even after successful treatment, reflecting years of endothelial damage and arteriosclerosis.
Left ventricular hypertrophy regresses slowly; echocardiographic evidence of improvement may not appear for 6-12 months. Patients with cardiomyopathy may require ACE inhibitors, beta-blockers, and sometimes cardiac resynchronization therapy as they recover.
Insulin sensitivity improves substantially after successful treatment, though frank diabetes may persist in those with irreversible beta cell loss. Weight loss, when achieved, further improves metabolic parameters.
Long-term mortality and cardiovascular event rates improve significantly after successful treatment compared to untreated disease. One large cohort study showed that 10-year survival was approximately 85% in treated patients versus 50% in untreated controls, with most excess deaths in the untreated group attributable to cardiac and cerebrovascular causes.
Practical Considerations for Patients
If you suspect Cushing's syndrome, or have been diagnosed, initiate frank conversations with your healthcare team. Ask about your cortisol levels, imaging findings, and the specific source of excess cortisol. Understand whether your case is ACTH-dependent or independent, and what treatment options are available.
Request baseline cardiac assessment: a standard ECG, a transthoracic echocardiogram, and blood pressure logs over several days. If you have hypertension, confirm whether it is difficult to control even on multiple agents. Discuss target blood pressure goals with your physician.
Before and after any surgical or medical intervention, ensure close follow-up. Cortisol recurrence can happen months or years later, particularly in pituitary-dependent disease. Annual or biannual cortisol measurement (24-hour UFC or late-night salivary cortisol) is prudent for long-term surveillance.
Be aware of potential complications of treatment. Post-operative pituitary insufficiency may require lifelong hormone replacement. Medical agents have side effects and require monitoring. Adrenalectomy necessitates glucocorticoid and mineralocorticoid replacement therapy for life.
Turquie Santé connects patients with specialist endocrinologists and cardiothoracic surgeons across Turkey's leading medical centers who have extensive experience managing Cushing's syndrome and its cardiac complications. Access to expert diagnosis and surgical treatment can be expedited through Turquie Santé's coordination services, ensuring you receive the specialized care this complex condition demands.