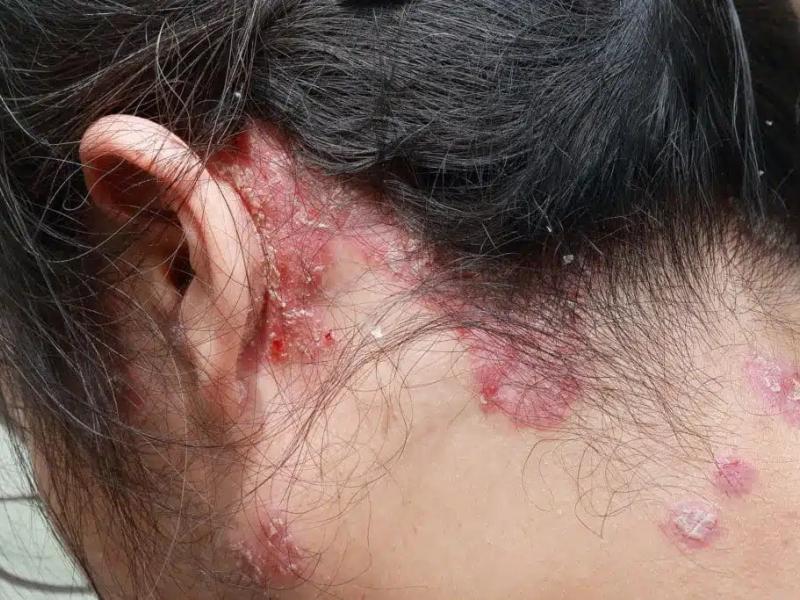
Scalp psoriasis is one of the most common manifestations of psoriasis, affecting the scalp with characteristic thick, silvery scales, persistent redness, and uncomfortable itching. This form of psoriasis stems from an autoimmune disorder where the body's immune system accelerates skin cell production, causing them to accumulate rapidly on the scalp's surface. Unlike general dandruff, scalp psoriasis creates well-defined patches that can extend beyond the hairline into surrounding areas.
What Makes Scalp Psoriasis Different From Other Scalp Conditions
Scalp psoriasis is fundamentally different from seborrheic dermatitis, though both cause scaling and itching. The distinction matters because treatment approaches differ significantly. Psoriasis patches tend to be thicker, more inflammatory, and less responsive to standard antidandruff shampoos. The scales in psoriasis are often silvery-white and tightly adherent to the skin, whereas seborrheic dermatitis typically presents with looser, yellowish scales.
The condition can manifest differently depending on the individual. Some people experience localized patches confined to a small area near the hairline or behind the ears. Others develop widespread involvement across the entire scalp, sometimes extending to the neck, forehead, and even the upper back. Severity fluctuates too. A patient might have mild itching and minimal scaling one season, then experience painful cracking and bleeding lesions during periods of stress or environmental triggers.
Common Symptoms and Clinical Presentation
Red, scaly patches represent the hallmark sign, typically appearing at the hairline margins, crown, or nape of the neck. Many patients report intense itching that worsens at night or during dry winter months. The scratching reflex often leads to secondary complications: small bleeding areas, crust formation, and temporary hair loss from mechanical trauma.
Beyond visible skin changes, patients frequently describe a sensation of tightness or discomfort across the scalp. This isn't merely cosmetic concern. The psychological impact of visible scaling, potential hair loss, and social embarrassment can be substantial. Some individuals experience flare-ups triggered by:
- Emotional stress or major life events
- Climate changes, particularly cold, dry winters
- Skin injuries or aggressive hair washing
- Certain medications or hormonal fluctuations
- Infection or bacterial colonization of the scalp
Scaling severity varies considerably. Mild cases produce only slight white flakes within the hair, easily dismissed as dandruff. Moderate-to-severe psoriasis generates profuse, thick accumulation that builds up visibly and may emit an odor if secondary infection occurs.
Accurate Diagnosis: Clinical Examination and Diagnostic Tools
Diagnosis typically begins with visual inspection and patient history. A dermatologist examines the scalp's appearance, noting the distribution, color intensity, and texture of lesions. The distinction between psoriasis and seborrheic dermatitis sometimes requires close observation, as early-stage psoriasis can mimic other conditions.
Dermatoscopy, a magnified examination technique, reveals characteristic vascular patterns specific to psoriasis: dilated capillaries arranged in a linear or tortuous pattern. This microscopic evidence helps confirm diagnosis when clinical appearance alone remains ambiguous.
Medical history provides crucial context. The physician inquires about:
- Symptom onset and progression timeline
- Family history of psoriasis or autoimmune conditions
- Recent triggering events: stress, infection, medication changes
- Previous treatments and their effectiveness
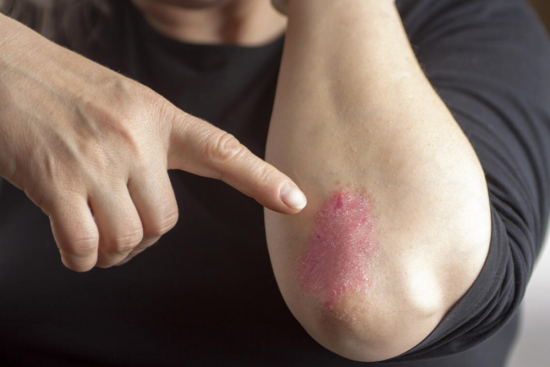
- Presence of psoriasis elsewhere on the body
If diagnosis remains uncertain, a small skin biopsy can be performed. Histopathology reveals the characteristic features of psoriasis: parakeratosis (retention of nuclei in the stratum corneum), acanthosis (thickened epidermis), and elongated dermal papillae with dilated vessels. Biopsy is rarely necessary for straightforward cases but proves invaluable when clinical presentation is atypical or when differential diagnosis between psoriasis and eczema remains problematic.
Treatment Options and Therapeutic Approaches
Management of scalp psoriasis typically follows a stepwise approach, beginning with topical agents and escalating to systemic therapy only when necessary. Treatment selection depends on severity, extent of involvement, patient age, and presence of systemic psoriasis.
Topical Treatments
Topical corticosteroids remain the first-line therapy for most cases. These reduce inflammation, suppress immune activity, and provide symptomatic relief relatively quickly. Potency levels range from mild (hydrocortisone) to ultra-potent formulations. For the scalp, healthcare providers typically prescribe moderate-to-potent steroids, such as betamethasone valerate or clobetasol propionate. Shampoo and lotion formulations penetrate the scalp better than creams.
Calcineurin inhibitors, including tacrolimus and pimecrolimus, offer a steroid-free option particularly useful for patients who cannot tolerate prolonged topical steroid use or have concerns about skin atrophy. These agents work by suppressing T-cell activation and may be combined with other treatments for enhanced effect.
Coal tar preparations have been used for decades. While effective, their messy texture and unpleasant odor limit compliance. Salicylic acid helps soften and remove scale buildup, often combined with other medications. Keratolytic shampoos containing tar or salicylic acid work by exfoliating dead skin, allowing better penetration of topical medications applied afterward.
Vitamin D analogues, such as calcipotriene, modulate skin cell differentiation and reduce inflammatory markers. These can be used alone or combined with topical corticosteroids, sometimes showing synergistic benefit.
Systemic and Biologic Therapies
When scalp psoriasis is severe, widespread, or accompanied by psoriasis elsewhere on the body, systemic medications become necessary. Methotrexate, a traditional immunosuppressant, effectively controls psoriasis but requires regular blood monitoring due to potential liver and bone marrow toxicity.
Biologic agents targeting specific immune pathways have revolutionized psoriasis treatment. TNF-alpha inhibitors (infliximab, etanercept), IL-17 inhibitors (secukinumab, ixekizumab), and IL-23 inhibitors (guselkumab, risankizumab) demonstrate remarkable efficacy in clearing psoriasis, including scalp involvement. These medications work by blocking inflammatory cytokines that drive the disease. Response rates vary; some patients achieve near-complete clearance while others see partial improvement.
Biologics require careful patient selection. Contraindications include active infections, malignancy risk, and certain cardiac conditions. Cost considerations and need for periodic infusions or injections also factor into treatment decisions.
Phototherapy
UVB phototherapy, particularly narrowband UVB (NB-UVB), can effectively treat scalp psoriasis, though accessing the scalp with standard phototherapy booths requires specialized equipment or home devices. Excimer laser therapy, targeting 308-nm wavelengths, concentrates treatment on affected areas and may achieve faster clearance with fewer systemic effects than whole-body phototherapy.
Practical Management and Lifestyle Modifications
Beyond medication, several practical strategies minimize flares and improve quality of life. Gentle hair care is fundamental. Harsh shampooing, vigorous brushing, and hot water damage the scalp barrier and provoke inflammation. Warm (not hot) water, sulfate-free shampoos, and soft-bristled brushes protect scalp health. Allowing sufficient drying time before brushing prevents mechanical trauma.
Stress management significantly influences disease activity. Meditation, regular exercise, adequate sleep, and counseling reduce stress-triggered flares in many patients. Identifying personal triggers, whether specific foods, weather patterns, or life events, enables preventive action.
Moisturization matters. Scalp psoriasis worsens in dry environments. Humidifiers, adequate hydration, and occasional scalp oils (coconut, jojoba) may provide comfort. However, heavy greasing can trap bacteria and worsen secondary infections.
Dietary considerations lack strong evidence, but some patients report improvement with anti-inflammatory diets emphasizing omega-3 fatty acids, reducing processed foods, and limiting alcohol. Individual responses vary tremendously.
When to Seek Advanced Care
Most scalp psoriasis responds adequately to topical therapy. However, consultation with a dermatologist becomes important if:
- Symptoms persist despite consistent topical treatment for 6-8 weeks
- Extensive scaling causes functional hair loss or significant distress
- Psoriasis extends beyond the scalp to the body, suggesting systemic involvement
- Secondary infection develops, manifesting as increased warmth, pus, or foul odor
- Topical steroids are ineffective or cause unacceptable side effects
Patients seeking treatment in Turkey can rely on dermatology services offered through Turquie Santé's partner clinics, which provide access to modern diagnostic techniques and comprehensive treatment protocols.
Long-Term Outlook and Disease Course
Scalp psoriasis is a chronic condition without cure, but it's highly manageable. Most patients achieve significant improvement or remission with appropriate treatment. Flares occur unpredictably; some individuals experience stable remission for months or years, while others deal with intermittent outbreaks.
The disease doesn't cause permanent scarring alopecia in most cases, meaning hair regrowth typically occurs once inflammation resolves. Complete hair loss from scalp psoriasis alone is rare; temporary shedding during active disease reflects inflammation rather than permanent follicle destruction.
Patient education and realistic expectations improve compliance and satisfaction. Understanding that psoriasis control requires ongoing maintenance therapy, that no single treatment works universally, and that cooperation with healthcare providers optimizes outcomes helps individuals navigate this chronic condition effectively.