Not everyone feels confident about their smile, and a gap between the front teeth can be a common reason why. Known as a diastema, this space can affect how you see yourself in photos or everyday moments.
The good news? A diastema is one of the easiest dental concerns to treat today. Whether the gap is small or more noticeable, modern dentistry offers effective solutions, from discreet aligners to natural-looking veneers.
In this guide, you’ll learn what causes a diastema, the treatment options available, and how to choose what’s right for you, so you can move forward with confidence.
What is a diastema?
A diastema is a gap or space between two adjacent teeth. The term is derived from the Greek word for "interval." While it can occur anywhere in the mouth, the most common and most visible form is the maxillary midline diastema (MMD): the gap between the two upper central incisors.
Clinically, a maxillary midline diastema is commonly defined as a space greater than 0.5 mm between the proximal surfaces of the central incisors, a threshold originally described by Keene and widely used in the literature. Smaller spaces may fall within normal anatomical variation or be considered aesthetically acceptable, depending on the clinical context and patient perception.
Is a diastema always a problem?
Not necessarily. In children, a midline gap is often a normal developmental stage during mixed dentition, the phase when baby teeth and permanent teeth coexist. In most children, this gap closes naturally once the permanent canines erupt and exert pressure on the incisors. No intervention is needed at this stage.
For adults whose gap has persisted beyond full eruption of the permanent dentition, treatment is primarily pursued for aesthetic and psychological reasons rather than purely functional ones. That said, larger diastemas can contribute to food trapping, gingival irritation, and certain speech articulation difficulties, giving treatment both cosmetic and health justifications.
Why do diastemas develop? Causes & differential diagnosis
Understanding the cause of your diastema is the most important step, because the cause directly determines the appropriate treatment. A thorough clinical evaluation should always precede any treatment plan.
1. Genetic & hereditary factors
Tooth size, jaw size, and the spacing patterns of teeth have a significant hereditary component. If your parents or siblings have gaps, you are statistically more likely to develop one. This type is often associated with a tooth-size/arch-size discrepancy, where the teeth are simply proportionally smaller than the space allocated for them in the jaw.
2. Abnormal labial frenum (frenal attachment)
The maxillary labial frenum is the small band of tissue connecting the inner surface of your upper lip to the gum tissue between the upper front teeth. When this frenum is unusually thick, fleshy, or extends deeply between the central incisors, inserting into the interdental papilla or even through to the palatal mucosa, it creates a physical barrier that prevents natural closure. This is known as a papilla-penetrating frenum, and it is one of the most well-documented causes of persistent midline diastema in adults.
3. Microdontia (undersized teeth)
When one or more teeth are smaller than average (microdontia), particularly the upper lateral incisors, which can sometimes be "peg-shaped", the dental arch has more space than the teeth fill, resulting in gaps throughout the anterior region.
4. Dental agenesis (missing teeth)
Congenital absence of a tooth (agenesis) leaves an unoccupied space in the arch. The most commonly absent permanent teeth are the upper lateral incisors, which, when missing, create significant spacing on either side of the central incisors.
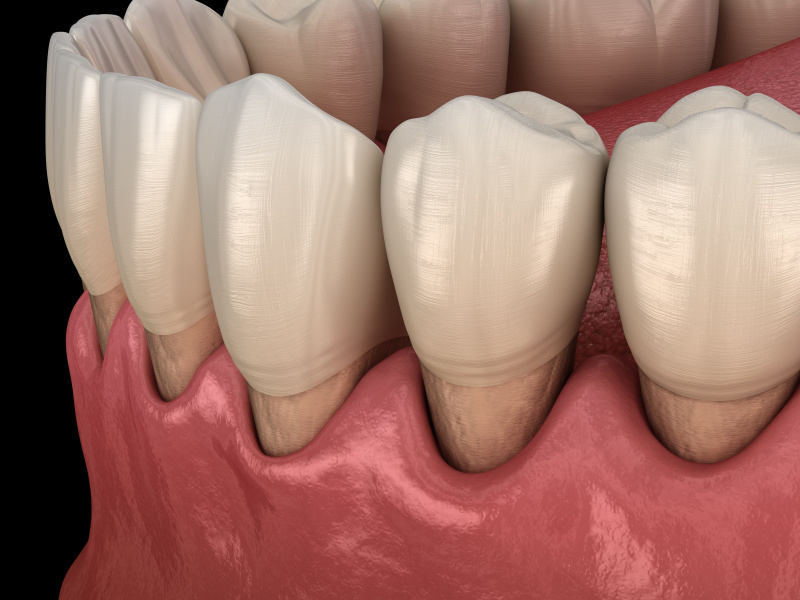
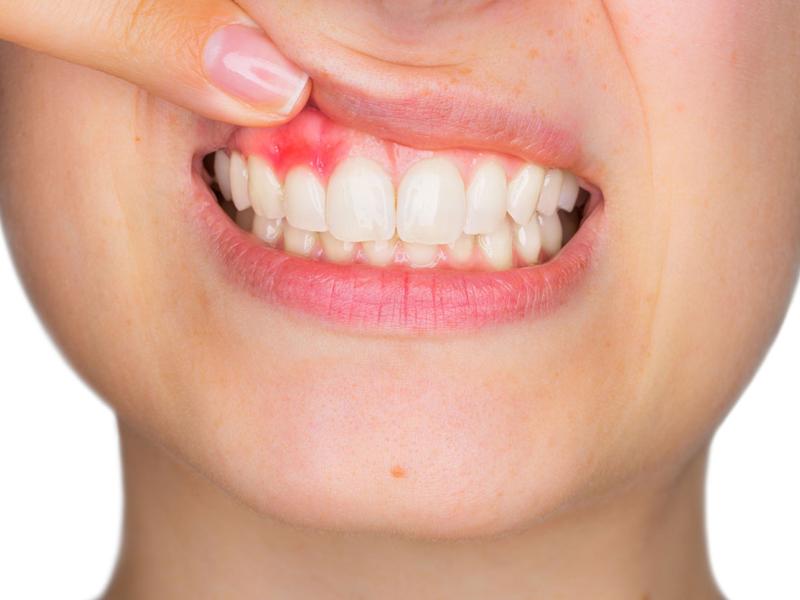
5. Periodontal (gum) disease
Advanced periodontitis causes destruction of the bone and ligament supporting the teeth. This loss of support can allow teeth to shift, tip, or drift, a phenomenon called pathological tooth migration, which can open or widen existing spaces. Diastemas that appear or worsen in adulthood, particularly in patients with bleeding gums, should always be evaluated for an underlying periodontal cause before any cosmetic treatment is attempted.
6. Parafunctional habits
Prolonged thumb-sucking or pacifier use in children exerts forward pressure on the upper incisors, tipping them outward (proclination) and widening interdental spaces. Tongue-thrusting, where the tongue pushes against the front teeth during swallowing, exerts similar forces.
7. Supernumerary teeth (mesiodens)
A mesiodens is an extra tooth located in the midline of the upper jaw, often impacted (unerupted) and invisible on external examination. It can physically block the central incisors from coming together and is diagnosable only through dental X-rays or CBCT imaging. Failing to identify and address a mesiodens will cause any orthodontic closure attempt to fail or relapse.
Consequences of an untreated diastema
A diastema is not a disease, but understanding its potential implications is important:
- Food impaction and gingival inflammation: Wider gaps can trap food debris. If oral hygiene is inadequate, this may contribute to gingival inflammation and increase the risk of caries in adjacent areas.
- Speech changes: Depending on the size and position of the gap, certain sounds—particularly “s,” “th,” and “f”—may be affected in some individuals.
- Psychological impact: Dental appearance can influence self-confidence and social interactions. Some patients with visible maxillary diastemas report feeling self-conscious about smiling, which may affect personal or professional situations.
- Possible progression: In cases related to periodontal disease or habits such as tongue thrusting, a diastema may increase in size over time if the underlying cause is not addressed.
Treatment options in Turkey: Choosing the right approach
Modern dentistry offers several well-validated options for closing or camouflaging a diastema. The best treatment depends on the cause, size of the gap, overall dental health, patient age, and aesthetic expectations.
There is no universal "best" option, each approach has specific indications, advantages, and limitations.
Fixed Orthodontic Appliances (Braces)
Traditional metal or ceramic brackets bonded to the teeth apply controlled forces to gradually close interdental spaces. Orthodontic treatment is the only approach that physically moves teeth to their correct positions, correcting the underlying alignment rather than masking it.
Best suited for: Large diastemas (> 2–3 mm), patients with multiple alignment issues, cases involving skeletal discrepancies, or when space redistribution across multiple teeth is needed.
Advantages:
- Addresses root cause, actually moves teeth
- Can correct multiple alignment issues simultaneously
- Predictable, well-documented outcomes
Limitations:
- Treatment duration: typically 12–24 months
- Fixed retainers required after treatment to prevent relapse
- Visible during treatment (though ceramic brackets are more discreet)
Important note on relapse: Orthodontic closure of a midline diastema, particularly one associated with an abnormal labial frenum, carries a risk of recurrence. A bonded lingual retainer (a thin wire glued to the back of the front teeth) is virtually always indicated after closure to maintain stability. Frenectomy may also be recommended in conjunction with orthodontic treatment.
Clear aligners (invisalign and similar systems)
Clear removable aligners, the most well-known brand being Invisalign, use a series of custom-fabricated transparent trays to apply incremental tooth movements. They are increasingly popular for diastema closure, particularly in adults.
The process: At the initial consultation, a digital intraoral scan (3D impression) is taken. Proprietary software generates a simulated treatment plan, and a series of custom trays are manufactured. Each tray is worn for approximately 1–2 weeks, shifting teeth slightly before progressing to the next tray.
Best suited for: Mild to moderate diastemas (< 3 mm) in patients who prioritize aesthetics during treatment and have good compliance.
Advantages:
- Nearly invisible
- Removable for eating and oral hygiene
- Fewer in-office appointments required
Limitations:
- Highly compliance-dependent, aligners must be worn 20–22 hours per day
- Less effective for complex tooth movements or significant skeletal issues
- Not suitable for active periodontal disease
Direct composite resin bonding
Composite resin is a tooth-colored dental material applied directly to the tooth surfaces to widen them and close the gap. It is sculpted, shaped, and polished chairside in a single appointment.
Best suited for: Small diastemas (< 2 mm), patients seeking a quick and cost-effective solution, or as a temporary measure.
Advantages:
- Single appointment
- Minimal or no tooth preparation
- Most cost-effective option
- Reversible
Limitations:
- Less color-stable than ceramic over time; susceptible to staining from coffee, tea, and red wine
- May require replacement after 5–7 years
- Less wear-resistant than porcelain
- Can appear bulky if the gap is large
4. Porcelain Laminate Veneers (PLVs)
Porcelain laminate veneers are ultra-thin ceramic shells, sometimes less than 0.5 mm thick, bonded to the front surface of teeth. For diastema closure, veneers are placed on both central incisors (and often lateral incisors), widening each tooth proportionally to close the gap.
A systematic review published in the Journal of Clinical Medicine reported a 10-year cumulative survival rate of approximately 95% for ceramic veneers, confirming their high long-term durability as a minimally invasive aesthetic treatment.
Modern lithium disilicate ceramics (such as IPS e.max) offer exceptional translucency and strength, closely mimicking natural tooth enamel.
Best suited for: Adults who decline orthodontic treatment or want faster results, cases involving microdontia, or patients who also want to improve tooth shape, color, or length simultaneously.
Advantages:
- Dramatic aesthetic transformation (often in 2–3 appointments)
- Highly color-stable and stain-resistant
- Long-lasting (10+ years with proper care)
- Can simultaneously address size, shape, and color
Limitations:
- Requires minimal enamel preparation (irreversible)
- More expensive than composite bonding
- Does not move teeth, camouflage rather than correction
- If the gap is too wide, closing it with veneers alone may create teeth that appear unnaturally wide
Key clinical consideration: When closing a diastema with veneers, careful space redistribution planning using diagnostic mock-ups or digital design is essential. The goal is to maintain a width-to-height ratio of approximately 72–85% for each tooth, the range associated with natural-appearing aesthetics.
5. Frenectomy (Labial Frenum Surgery)
When an abnormal labial frenum is identified as the primary cause of the diastema, or a contributing factor preventing orthodontic closure, a frenectomy may be recommended. This is a minor surgical procedure to remove or reposition the frenal tissue.
Important clinical nuance: Frenectomy alone rarely closes a diastema. Current evidence strongly indicates that frenectomy is most effective when performed in conjunction with orthodontic treatment, not as a standalone solution. The timing of the procedure relative to orthodontic treatment is a matter of clinical judgment:
- Performing the frenectomy during orthodontic treatment (once space closure is near complete) is generally preferred, as the resulting scar tissue can help stabilize closure while space is still controlled.
- Performing frenectomy before orthodontic treatment risks creating scar tissue that may impede subsequent tooth movement.
- Performing it after treatment carries a relapse risk if the frenum is not addressed.
A survey of UK orthodontists found that approximately three-quarters would consider frenectomy as part of orthodontic treatment for maxillary midline diastema closure rather than as a standalone procedure. The study also highlighted a lack of consensus regarding timing, reinforcing its role as an adjunct rather than a primary treatment modality (Ahn et al., The Angle Orthodontist, 2022).
Modern frenectomy is performed with a conventional scalpel, electrocautery, or increasingly with diode or Er:YAG laser, the latter offering reduced postoperative discomfort, minimal bleeding, and faster healing.
Comparing Treatment Options: A Quick Reference
| Treatment | Gap size | Duration | Permanence | Invasiveness | Best for |
| Braces / Fixed Appliances | Any size | 12–24 months | Permanent (with retainer) | Non-invasive | Complex cases, multiple alignment issues |
| Clear aligners | Small–moderate | 6–18 months | Permanent (with retainer) | Non-invasive | Mild gaps, adults, aesthetics-conscious |
| Composite bonding | Small (< 2 mm) | 1 appointment | 5–7 years | Minimal | Quick fix, budget-conscious |
| Porcelain veneers | Small–moderate | 2–3 appointments | 10–15+ years | Minimal enamel prep | Adults, fast results, also improving aesthetics |
| Frenectomy | N/A (adjunct) | 1 appointment | Permanent | Minor surgery | Frenum-related diastemas, prevents relapse |
Why choose Turkey for diastema treatment?
Turkey, especially Istanbul, has become a top destination for dental care, attracting patients from around the world. And it’s not just about lower prices:
- Affordable treatment: Dental care in Turkey typically costs 50–70% less than in the UK, Germany, or the US, mainly due to lower operating costs—not lower quality.
- Modern clinics: Many dental centers use advanced technologies such as digital scanners and CAD/CAM systems, with dentists often trained internationally.
- All-in-one care: Clinics usually offer complete treatment plans, combining orthodontics, gum care, and cosmetic procedures in one place—ideal for more complex cases.
- Trusted standards: Reputable clinics follow international standards and work with qualified, registered specialists.
Prevention: Can you prevent a diastema?
Some causes of diastema, such as genetics and natural tooth size, are beyond our control. However, the following measures can reduce modifiable risk factors, particularly in children:
- Discourage thumb-sucking and pacifier use beyond age 3–4, as prolonged habits can tip the front teeth forward and widen interdental spaces.
- Address tongue-thrusting habits with the help of a myofunctional therapist if identified.
- Maintain good periodontal health, regular dental cleanings and early treatment of gum disease prevent pathological tooth migration.
- Early orthodontic evaluation at age 7–8 allows a specialist to identify developing issues (including mesiodens or abnormal frenum) before they become more complex to treat.
Ultimately, while not all diastemas can be prevented, early awareness, good oral habits, and timely professional care play a key role in minimizing their development and ensuring optimal long-term dental health and aesthetics.